The couple needs to overcome their infertility problems which leads to discussions about the woman in the relationship. The discussion focuses on testing and reproductive cycles and the established timeframes. Most couples discover this fact after their attempt to conceive which shows that male infertility causes conception problems in almost half of all delayed cases. Varicocele and male fertility are closely linked because varicocele which causes scrotal veins to expand is one of the main but undeservedly ignored factors that leads to male infertility because it affects sperm health and hormonal balance which decreases the likelihood of natural conception.
Dr. Aravind's IVF Fertility and Pregnancy Centre operates 40+ branches throughout Tamil Nadu and Karnataka and Kerala and Andhra Pradesh to help couples who have not been informed about their male partner's treatable condition that prevents them from becoming parents and provides varicocele treatment in Coimbatore and across South India. With proper diagnosis and timely treatment doctors can effectively treat patients who have varicocele because this condition requires medical intervention to solve the problem.
The article serves men whose semen analysis male fertility results show suboptimal results and couples who seek additional treatment options and people who want to learn about varicocele's impact on male reproductive health.
The veins inside the scrotum function as a waste removal system which operates to remove blood from the testicles after the blood has provided essential nutrients and oxygen to the testicles. The veins in the body experience blood accumulation when their internal valves malfunction because the normal blood circulation pattern gets disrupted. The veins develop bulging and twisting patterns that resemble varicose veins, which appear on human legs because of this blood accumulation, defining varicocele symptoms.
Varicocele occurs with high frequency because it affects both sexes. It is found in approximately 15% of all men and in nearly 40% of men who are investigated for primary infertility, highlighting that varicocele can cause infertility. The secondary infertility rate, which applies to couples who experienced a previous pregnancy but now face challenges in conceiving again, displays an even greater occurrence of the condition.
The condition primarily affects the left side of the scrotum. The left testicular vein connects to the renal vein by draining at a right angle, which makes this anatomical structure vulnerable to developing high venous pressure. The medical condition of bilateral varicocele, which affects both sides of the body, occurs frequently and results in greater damage to testicular function and sperm production capacity.
Testicles function as temperature-sensitive body parts because they require an environment that maintains a temperature which falls below normal body heat. The scrotum exists as an exterior body part for this precise purpose. The varicocele condition causes blood to accumulate in veins which increases scrotal heat and this temperature change functions as a major factor which prevents men from becoming fertile and explains how varicocele affects sperm quality.
The body experiences oxidative stress because damaged veins prevent normal blood flow which results in free radicals exceeding the capacity of antioxidants to fight them. These free radicals attack sperm cells and cause damage which decreases their ability to move and changes their physical structure while breaking apart their genetic material leading to DNA fragmentation sperm issues.
Elevated sperm DNA fragmentation has become widely accepted as an undiscovered cause behind IVF failure and recurrent miscarriage which occurs despite normal semen test results.
Varicocele produces disruptions to the hormonal system which controls male reproductive capabilities. The hormone testosterone experiences a drop in levels while testosterone and estradiol ratios undergo an unfavorable shift which contributes to hormonal imbalance male fertility issues.
Men who have large varicoceles which affect both testicles will experience gradual testicle size loss because their condition remains untreated. This matter holds special significance for younger men and adolescents because medical professionals can help them keep their ability to reproduce throughout their lives.
The knowledge of varicocele requires people to know that it commonly shows no symptoms. Men with this condition remain undiagnosed for multiple years because they remain unaware of its presence. The condition usually gets detected during fertility assessments or standard medical checkups for male infertility causes.
The first symptoms of the condition create a dull ache that becomes heavier in the left testicle after men spend extended time standing or exercising or after they complete their daily activities. Some men describe the sensation as a dragging discomfort that occurs in their scrotum, which are common varicocele symptom.
Self-examination reveals a feeling of lumps that create a 'bag of worms' texture that becomes more pronounced with larger varicoceles.
The pain that occurs is often treatable because it does not reach an extreme level of intensity. The condition becomes more severe in warm temperatures while it gets better when a person rests in a position that relieves gravitational force from their veins. The signs that you recognize from this list should undergo assessment because the condition may cause infertility issues that you do not yet recognize despite the absence of painful symptoms.
Effective treatment requires dependable diagnostic results as its essential base. Dr. Aravind's IVF uses clinical expertise and advanced diagnostic tools to deliver complete and precise varicocele diagnostic results.
Our centres use Doppler ultrasound as a standard practice to assess male fertility in cases where semen results fall below established thresholds or when couples have experienced unsuccessful attempts to conceive for more than twelve months.
Not every varicocele requires treatment. The decision to intervene depends on several factors: the grade of the varicocele, the man's sperm production capacity, existing medical symptoms and the couple's current efforts to achieve pregnancy. The primary treatment goal aims to stop abnormal venous reflux, decrease scrotal temperature and establish conditions that will boost sperm production. The following are the main treatment approaches available today.
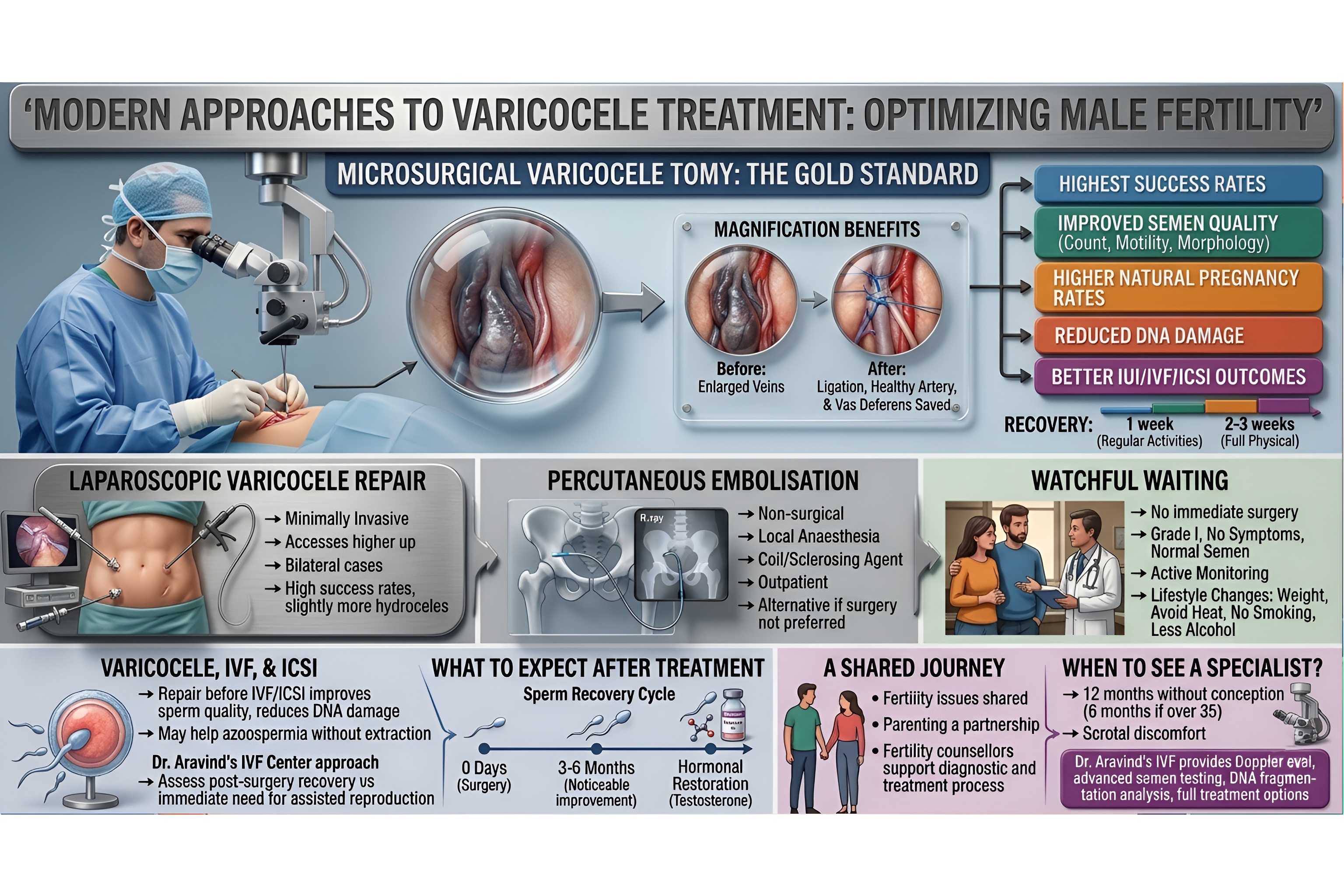
This method currently stands as the most successful surgical option to treat varicocele and it serves as the main treatment method used by top fertility clinics throughout the world. During microsurgical varicolectomy the surgeon creates a minor cut either in the groin area or below it to conduct the procedure through an operating microscope which enables him to see and tie off the enlarged veins while keeping the testicular artery and lymphatic system and vas deferens safe.
This technique uses magnification to achieve its main distinctive feature. The method achieves this outcome through hydrocele formation which refers to the build-up of fluid around the testicle and through the recurrence of the varicocele. Most men can start their regular activities again after one week of recovery while they need two to three weeks for complete recovery of their physical capabilities.
Studies show that microsurgical varicocelectomy improves semen quality because most men experience better sperm count and motility and morphological development in their semen. Natural pregnancy rates after the procedure show significant results. Improved sperm quality after surgery results in better outcomes for IUI and IVF with ICSI even when natural conception does not happen.
The surgical procedure of laparoscopic varicocelectomy requires general anaesthesia for its minimally invasive technique. The surgeon uses a small camera and instruments inserted through tiny abdominal incisions to access and ligate the affected veins higher up in the abdomen. This approach provides an effective treatment solution for bilateral varicocele cases because both sides of the condition can be treated through the same surgical openings. The laparoscopic repair method achieves high success rates but results in slightly more cases of hydrocele development than the microsurgical method.
Percutaneous embolisation is a radiological non-surgical procedure that uses a catheter to enter through a vein at either the groin or neck which doctors control with X-ray imaging to deliver a coil or sclerosing agent for abnormal vein obstruction treatment. The procedure enables patient treatment without surgical incision requirements because it only needs local anaesthesia to complete and the patient can leave the clinic after their treatment. The procedure serves as an effective treatment solution for men who do not meet surgery requirements or choose to avoid surgical treatments. The method shows slightly decreased success rates when compared to microsurgical varicocelectomy according to some studies which show restricted access to the procedure.
Men with varicocele do not require immediate surgical treatment as their condition needs evaluation. The couple needs active monitoring when their Grade I varicocele shows no symptoms and their semen parameters remain normal and they maintain a healthy weight. The patient can support sperm health through lifestyle changes which include maintaining a healthy weight and avoiding prolonged heat exposure to the groin and quitting smoking and reducing alcohol intake during the clinical observation period.
The centers receive frequent inquiries about whether varicocele treatment should proceed before IVF or ICSI when these procedures are planned anyway. The answer, in most cases, is yes and for good reason. The process of varicocele repair before IVF or ICSI treatment leads to significant improvements in sperm quality which reduces DNA damage and decreases the number of treatment cycles needed to achieve successful conception.
The surgical treatment of varicocele enables men with extreme sperm deficiencies who suffer from severe oligospermia and azoospermia to achieve sperm recovery through natural means instead of needing testicular sperm extraction. Couples who have an older female partner need to evaluate their situation with a more detailed examination of their decision-making process.
The fertility specialists at Dr. Aravind's IVF center assess all cases through a process which evaluates the duration needed for post-surgical sperm recovery and compares it to the immediate requirement of performing assisted reproduction. The ideal solution for each couple exists as the most suitable option that requires proof for their specific situation.
The first question most men ask after varicocele surgery is: 'When will my sperm show signs of improvement?" The production of sperm occurs through a process which takes about 72 to 90 days to complete its entire cycle. After a successful operation, patients will start to notice significant changes in their semen measurements between three and six months after the procedure.
The post-operative period includes scheduled follow-up tests which will evaluate semen production to assess how well the patient is progressing through recovery. Most men experience progressive increases in both sperm count and sperm movement abilities while their DNA damage levels decrease. The body undergoes hormonal restoration which includes testosterone levels reaching their normal levels according to men whose energy and sexual desire along with overall health status improved.
People need to understand that they should create goals which they can achieve within their abilities. The procedure will benefit some men through better results whereas other men will achieve natural conception through repaired varicoceles. The majority of men who start treatment after they reach the point of permanent testicular damage will experience positive outcomes. At Dr. Aravind's IVF, our andrologists and embryologists work together to monitor progress and adjust the fertility plan at each stage of recovery.
Couples share the experience of fertility difficulties which can develop from either partner's reproductive problems. Our clinic at Dr. Aravind's IVF holds the view that parenting requires a collaborative relationship between partners who should progress through the journey together. A man who receives a varicocele diagnosis experiences an unexpected burden that he believes he must face without support.
The situation does not require such an outcome.Our fertility counsellors work with both partners to ensure that every step of the diagnostic and treatment process is understood, supported, and approached together. Our team across all our centres in South India will provide you with clinical expertise and compassionate support during your upcoming surgical procedures and assisted reproduction treatments.
The couple needs to complete a full fertility assessment which includes testing for male partners after they have failed to conceive for 12 months or six months if the woman is over 35. You should visit a doctor if you experience discomfort in your scrotum because you have not yet attempted to conceive. Early diagnosis of varicocele protects your fertility potential before irreversible damage has a chance to occur.
Dr. Aravind's IVF provides complete male fertility services through their Doppler evaluation and advanced semen testing and DNA fragmentation analysis and their comprehensive surgical and reproductive treatment methods which enable them to deliver full partner care at all treatment phases.
Varicocele is the enlargement of veins in the scrotum, similar to varicose veins, which can affect sperm production and fertility.
Yes, varicocele can impair sperm quality, motility, and DNA integrity, leading to male infertility.
Symptoms may include scrotal pain, swelling, a “bag of worms” feeling, or no symptoms at all.
Diagnosis is done through physical examination, Doppler ultrasound, semen analysis, and hormone tests.
Microsurgical varicocelectomy is considered the most effective treatment with high success rates.