Most couples in India and throughout the world face challenges during their quest to become parents. Modern assisted reproductive technology (ART) provides couples with a vital solution when they face challenges with natural conception because the system needs one essential choice, which functions as the foundation for successful ART outcomes. Magnetic-Activated Cell Sorting, which scientists developed as a method to select sperm, represents one of the most advanced sperm-selection methods because it enables users to observe details that exceed basic microscope capabilities. This makes MACS sperm selection for ICSI an increasingly preferred option in modern ICSI treatment in India, especially in cases of male factor infertility
Dr. Aravind's IVF Fertility & Pregnancy Centre provides advanced fertility solutions to couples through its three decades of medical expertise and its accomplishment of more than 70000 IVF procedures. Our embryology team uses MACS as a specialized method during Intracytoplasmic Sperm Injection (ICSI) cycles when we need to evaluate sperm DNA damage. This article provides an explanation of MACS through basic language, which describes its operation mechanism and its significance to people who will gain advantages from its use and its relationship to the complete field of fertility treatment.
The technique of ICSI (intracytoplasmic sperm injection) is where a single sperm is chosen and then microinjected directly into an egg that has already been made mature. This procedure enables men who have extremely low sperm production or who have poor sperm movement or abnormal sperm shape to become fathers of their own biological children. ICSI treatment results depend entirely on the necessary sperm quality, which must be chosen for treatment. This is why identifying the best sperm selection technique ICSI, is critical for improving outcomes, particularly in male factor infertility treatment. The challenge of sperm DNA assessment exists because both patients and some doctors make the mistake of thinking that standard microscopic examination will show all sperm abnormalities. Sperm with fragmented or deteriorated DNA may successfully fertilize an egg, but the resulting embryo is often of poor quality. Couples who dedicate all their emotional and financial resources to treatment face three outcomes, which include failed implantation combined with early miscarriage and unsuccessful IVF cycles.
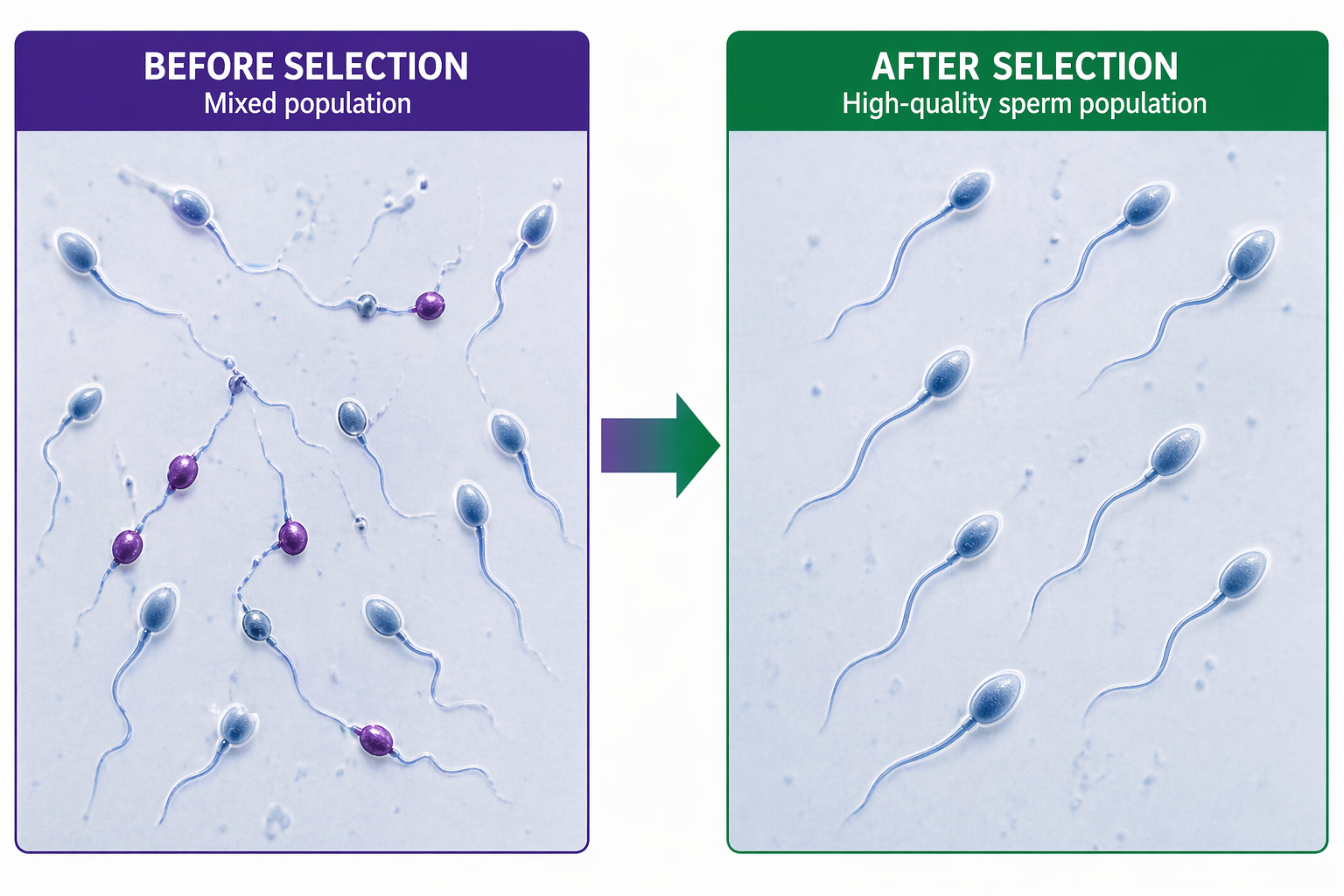
The solution to this problem exists because MACS was created to address it. The laboratory technique of Magnetic-Activated Cell Sorting uses magnetic fields to search for and remove sperm that have started to undergo programmed cell death, which scientists call apoptosis. This process is especially useful as a sperm DNA fragmentation treatment strategy in assisted reproduction. The removal of apoptotic sperm before ICSI creates a better sperm pool, which becomes available for fertilization.
The study of MACS requires knowledge of the biological marker phosphatidylserine (PS). In a healthy cell, this phospholipid molecule exists on the inner membrane layer of the cell membrane. The sperm cell starts its self-destruction process through early apoptosis when phosphatidylserine moves from the inner membrane to the outer membrane. The externalized PS functions as a biological indicator that shows that "This cell is damaged."
The MACS system utilizes Annexin V protein, which naturally binds to externalized phosphatidylserine with strong force. The MACS process uses Annexin V, which scientists apply to magnetic nanoparticles that exist as invisible beads, which are smaller than the human eye's range of vision. The magnetic bead-Annexin V complexes attach to apoptotic sperm, which show phosphatidylserine on their outer surface, when the prepared semen sample comes into contact with these complexes.
The molecular precision of MACS functions as its primary operational mechanism. The system detects dying sperm through its cellular and genetic testing, which includes both visual assessments of sperm shape and movement.
Research evidence demonstrates that MACS shows positive results in ART for certain patient groups. Studies evaluating MACS ICSI success rates suggest improved pregnancy outcomes compared to traditional methods. A systematic review and meta-analysis published in a peer-reviewed reproductive medicine journal found that sperm selection using MACS resulted in statistically significant improvements in pregnancy rates when compared to density gradient centrifugation and swim-up techniques alone, with a 50 percent increase in pregnancy success through MACS based on a 1.50 relative risk.
Clinical research has demonstrated that MACS-selected sperm lead to reduced miscarriage rates in autologous ICSI cycles and increased pregnancy success in egg-donation cycles and substantial live-birth rate improvement across both cycle types. The research showed that couples with high sperm DNA fragmentation (SDF) benefit from MACS because it lowers damaged sperm levels while transforming DNA fragmentation index values from above 30 percent down to below 8 percent which determines whether a pregnancy will succeed or fail.
The research shows that MACS-selected samples produce better sperm morphology results and greater progressive motility rates when compared to traditional sample preparation methods. The combination of MACS and density gradient centrifugation enables researchers to achieve a recovery rate of 68% for progressively motile sperm, while unprocessed ejaculate achieves only 39% recovery.
The research requires transparent disclosure because different studies produce different results for various patient groups. In couples without significant sperm DNA damage or apoptosis issues, the added benefit of MACS over standard preparation may be marginal. The IVF clinic at Dr. Aravind requires personalized assessment by a specialist fertility team to determine the actual need for MACS treatment.
MACS is not required for every ICSI cycle, but it can be a game-changer for certain groups of patients. The fertility specialists at Dr. Aravind's IVF facility establish MACS as an essential component of ICSI protocols when they identify the following conditions in their patients.
The advanced paternal age of men undergoing ICSI leads to sperm quality decline. Older men who undergo ICSI should use MACS to enhance their selected sperm quality during fertilization. MACS helps mitigate these effects as part of advanced sperm selection IVF techniques.
The advanced sperm selection methods that modern IVF laboratories offer serve as the basis to evaluate MACS through its position in their complete advanced sperm selection system. The different techniques present various benefits that match specific medical situations.
Dr. Aravind's IVF facility has established its operation for its embryologists to follow customized procedures instead of standardized methods. Our experts evaluate your complete fertility history together with semen analysis and sperm DNA fragmentation test results to identify the treatment method that will give you the highest chance of success through standard and advanced techniques.
Dr. Aravind's IVF clinic places patient safety above all other concerns because couples need to understand the risk factors associated with each laboratory test they want to undergo. The MACS system operates with complete safety because it demonstrates high safety performance according to testing results. The published clinical literature does not report any side effects that occurred during the MACS procedure. The magnetic nanoparticles and Annexin V used in the procedure do not come into contact with the egg during fertilization — MACS acts entirely on the sperm sample before injection.
The birth defects and developmental problems of children born through MACS-assisted ICSI show no increase when compared to children born through standard ICSI. The procedure itself takes place within the embryology laboratory and adds only a modest amount of processing time to the standard ICSI workflow.
The method used by MACS to remove damaged sperm from the sample, instead of changing healthy sperm, allows the system to function with human biology. The MACS system extracts sperm, which represents the highest potential for natural fertilization success.
The Dr. Aravind IVF Fertility and Pregnancy Centre has established itself as the leading reproductive medical centre in India since its founding more than 30 years ago. Our centres have achieved a success rate of 75% live births through more than 70000 completed IVF cycles, which have established our centres in Tamil Nadu, Kerala, and Karnataka as reliable facilities for families who considered parenthood impossible.
Our advanced sperm selection approach through MACS testing demonstrates our main belief, which states that every couple requires a customized fertility strategy that matches their specific biological, historical and personal requirements. We do not recommend expensive or complex procedures simply for the sake of it. The team of experienced embryologists and fertility specialists will assess your case to determine whether MACS will enhance your results.
They will provide complete details about the process, its benefits and upcoming developments. The latest technology serves as our lab foundation while our embryologists receive ongoing education to master advanced methods, which include MACS, IMSI, PICSI and AI-assisted embryo selection. The combination of the latest scientific advancements, together with our deeply compassionate approach, drives couples with complex fertility problems to trust Dr. Aravind's IVF facility.
The experience of becoming a parent represents one of the most significant human life paths. The proper technological solutions, together with an effective team, create success during difficult times. Modern fertility medicine uses MACS as a demonstration of its precise scientific capabilities because the method identifies sperm with maximum genetic integrity through molecular analysis. At Dr. Aravind's IVF, our facility operates through scientific advancements, which we combine with our authentic dedication to providing compassionate healthcare for each couple we serve. Recognized as one of the best IVF centres in Chennai, the clinic offers cutting-edge solutions tailored to each patient.
Our team recognizes that every consultation, together with every treatment cycle and every outcome, brings substantial emotional impact to our clients. The 20000 successful births we achieved serve as our motivation to develop our facility with state-of-the-art medical technologies. Our team also provides transparent guidance on ICSI treatment cost in India and additional procedures, such as MACS sperm selection cost, ensuring patients can plan financially with clarity.
We welcome you to schedule a consultation with our experts if you want to learn about MACS and other advanced sperm selection methods after your ICSI treatments or previous fertility treatments did not succeed. We provide all the necessary support to help you achieve your goal of becoming a parent.
MACS filters out sperm with DNA fragmentation, improving embryo quality, increasing implantation chances, and reducing miscarriage risk.
MACS is recommended for men with high sperm DNA fragmentation, repeated IVF/ICSI failures, poor embryo quality, or advanced paternal age.
Yes, MACS is considered safe. The process only acts on sperm before fertilization and does not affect the egg or embryo.
No, MACS improves sperm quality but does not guarantee pregnancy. Success depends on multiple factors including egg quality and overall health.
MACS targets sperm at a molecular level by removing apoptotic cells, while IMSI focuses on morphology and PICSI evaluates sperm maturity.