For years, people believed that IVF success came down to just two things: a healthy embryo, which acts as the seed, and a welcoming uterine lining that functions like fertile soil. Even when embryos appeared healthy and the uterine lining looked perfect in medical evaluations, many couples still left fertility clinics without clear answers or successful outcomes. This experience has been emotionally challenging for many patients seeking fertility treatment.
Today, scientific understanding of fertility has evolved. Researchers have discovered that the uterus is not a sterile or empty environment as once believed. Instead, it contains a small but important community of microorganisms known as the uterine microbiome. These bacteria play a significant role in reproductive health and may influence whether an embryo successfully implants or fails to develop.
Similar to how gut health affects overall well-being, the balance of bacteria within the uterus can impact the success of fertility treatments. A healthy microbial environment helps support implantation, while an imbalance in these microorganisms may contribute to implantation failure or unexplained infertility.
This guide explores this emerging area of reproductive science. We will examine how gut health, vaginal microbiota, and the uterine microbiome are interconnected and how these factors may influence your IVF journey and overall fertility outcomes.
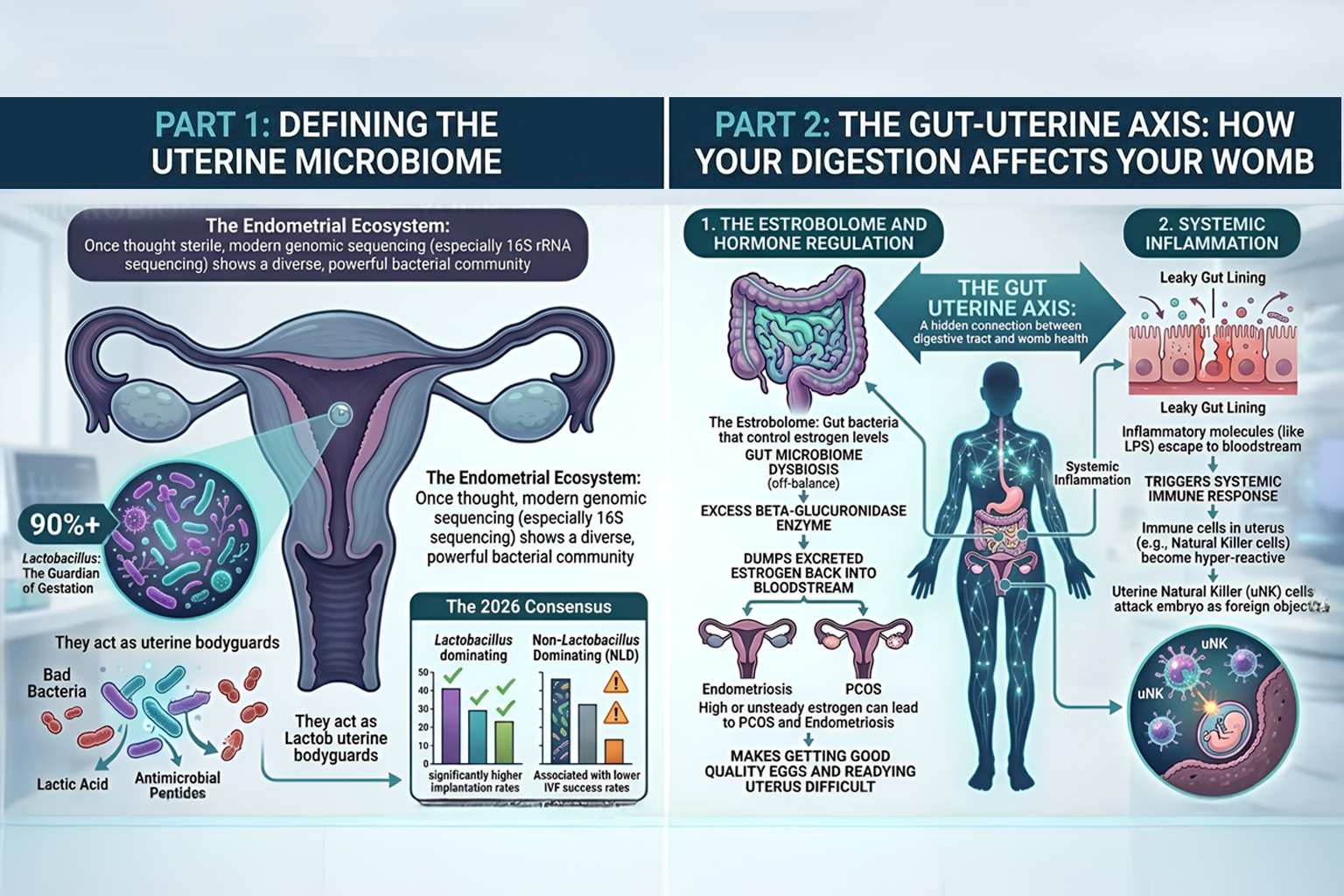
For many years, medical science believed the uterus was completely sterile. However, modern genomic technologies such as 16S rRNA sequencing have changed this understanding. Research now shows that the uterus contains a small yet highly influential community of bacteria known as the uterine microbiome. These microorganisms play an important role in maintaining a healthy reproductive environment and can directly influence embryo implantation and pregnancy outcomes.
A healthy uterine microbiome is typically dominated by beneficial bacteria known as Lactobacillus. In most successful reproductive environments, these bacteria make up more than 90% of the microbial population within the uterus.
Recent fertility research suggests that a Lactobacillus-dominated uterine environment is strongly associated with higher implantation rates, improved live birth outcomes, and lower miscarriage risk when compared with a Non-Lactobacillus Dominated (NLD) microbiome.
The gut–uterine axis refers to the biological connection between gut bacteria and reproductive health. The microorganisms in your digestive system can influence hormone balance, immune responses, and inflammation levels throughout the body—including the uterus. Because of this connection, digestive health can significantly impact fertility and IVF success.
When the uterine microbiome is not dominated by Lactobacillus, harmful bacteria such as Gardnerella, Streptococcus, or Enterococcus may become more prevalent. This imbalance can create an inflammatory environment that interferes with successful embryo implantation.
Chronic Endometritis (CE) is a persistent low-grade inflammation of the endometrial lining caused by bacterial infection. Unlike acute infections, CE often produces few or no symptoms, which makes it difficult to detect without specialized testing.
Modern fertility treatments increasingly include microbiome testing to understand the bacterial environment within the uterus. These tests help fertility specialists identify potential issues that may affect implantation success.
Improving the uterine microbiome is possible with a comprehensive approach that focuses on gut health, vaginal microbiota, and lifestyle factors. A structured three-month protocol can significantly improve microbial balance before IVF treatment.
Modern reproductive medicine is shifting away from a one-size-fits-all IVF approach. Personalized fertility care now includes evaluating and optimizing the uterine microbiome before embryo transfer. By understanding the connection between the gut, vaginal microbiota, and the uterine environment, fertility specialists can create more effective treatment strategies for patients experiencing unexplained infertility or repeated implantation failure.
Successful IVF treatment is not determined solely by laboratory procedures. The health of the uterine environment plays a crucial role in whether an embryo implants and develops into a healthy pregnancy. Understanding the relationship between gut health and reproductive health empowers patients to take a proactive role in their fertility journey.
For individuals experiencing recurrent IVF failure or conditions such as PCOS or endometriosis, evaluating the microbiome may provide valuable insights into hidden fertility challenges. By optimizing the body's internal environment, couples can improve their chances of achieving a successful pregnancy.
For many years the uterus was believed to be sterile, but modern genetic sequencing has shown that a small but important group of microorganisms exists there. A healthy uterine microbiome is usually dominated by Lactobacillus bacteria which help maintain a protective environment that supports embryo implantation and pregnancy.
The uterine microbiome plays a significant role in embryo implantation and pregnancy outcomes. When the uterus has a Lactobacillus-dominant environment, implantation rates and live birth rates are generally higher. However, if harmful bacteria dominate the microbiome, inflammation may occur, making it harder for the embryo to attach to the uterine lining during IVF.
The gut-uterine axis refers to the connection between gut bacteria and reproductive health. The microorganisms in the digestive system influence hormone balance, immune responses, and inflammation levels. Because of this connection, an unhealthy gut microbiome may indirectly affect the uterine environment and reduce the chances of successful implantation during IVF.
Yes, gut health can influence fertility in several ways. The gut microbiome helps regulate hormones such as estrogen through a group of bacteria known as the estrobolome. When gut bacteria become imbalanced, hormone levels may fluctuate and increase inflammation in the body. These changes can make the uterine environment less favorable for embryo implantation.
Chronic endometritis is a persistent, low-grade inflammation of the uterine lining caused by certain bacteria. Unlike acute infections, it often produces no obvious symptoms. Research shows that a significant percentage of women experiencing recurrent implantation failure during IVF may have chronic endometritis. Treating this condition can improve the chances of successful implantation.