The IVF procedure starts with scientific work, which needs exact timing and constant observation. The most important equipment that fertility doctors need during their work is ultrasound technology. The whole process of IVF monitoring through ultrasound procedures extends beyond basic scanning because it enables doctors to track and quantify all clinical activities, which start with ovarian stimulation and continue until doctors transfer embryos.
The practitioners at Dr. Aravind's IVF Fertility and Pregnancy Centre use their three decades of medical expertise and their experience of performing more than 70000 IVF procedures through their advanced ultrasound equipment to develop custom treatment plans that deliver maximum success rates.
The article provides a complete explanation of ultrasound monitoring, which includes its purpose in different stages and what patients will experience during their medical visits.
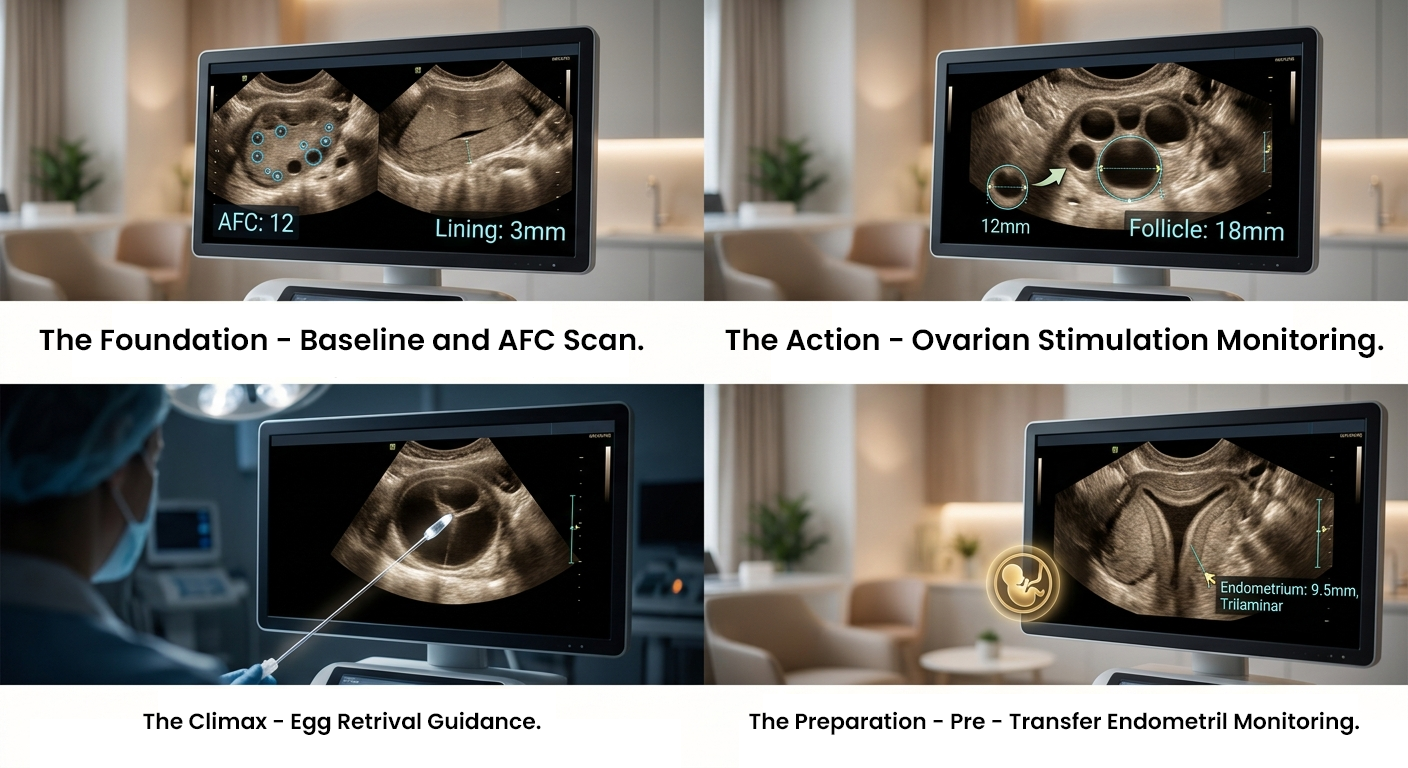
IVF ultrasound monitoring refers to the ongoing application of high-definition ultrasound technology, which most commonly uses transvaginal ultrasound for tracking reproductive organ development throughout a treatment cycle. The scans deliver immediate visual data about the ovaries and follicles, which are fluid-filled sacs that contain eggs and the uterine lining, endometrium.
IVF monitoring scans develop their own measurement system, which differs from the ultrasound scans you received during your pregnancy. Doctors monitor follicle development by measuring the number of follicles that grow, their size increase and their speed of growth, and they assess endometrial thickening, which results from hormone treatment.
The transvaginal ultrasound (TVS) stands as the primary examination technique that uses a small, smooth probe for precise pelvic organ imaging through vaginal insertion. This method achieves better imaging results than abdominal scans while patients experience high levels of comfort during the process.
IVF does not provide a universal solution because it requires individualized treatment. The hormone doses used to stimulate the ovaries must be tailored to your individual response — and that response can only be measured accurately through regular ultrasound scans combined with blood hormone tests.
The IVF treatment process requires this particular monitoring process because it establishes treatment paths based on medical evidence. The presence of this system enables fertility specialists to make treatment choices that rely on medical evidence throughout their work.
Your doctor will conduct a baseline ultrasound examination on day 2 or day 3 of your menstrual cycle before any fertility medications are approved for prescription. Your initial ultrasound assessment establishes the basis for your whole treatment schedule.
The doctor will perform several tasks during the baseline scan.
The AFC serves as a key indicator that predicts the effectiveness of ovarian response to stimulation drugs. The higher count provides a stronger response indication, while the lower count requires protocol changes and increased patient observation.
Monitoring Scans During Ovarian Stimulation
Your monitoring schedule begins after your stimulation injections start, which usually occurs between the second and fifth days of your menstrual cycle. Your IVF monitoring schedule depends on these appointments, which give patients their best opportunity to observe their developing eggs.
Under stimulation conditions, follicles show a daily growth rate that ranges from 1 millimetre to 2 millimetres. The doctor wants to observe a group of follicles that develop at the same speed, which will achieve a size between 17 millimetres and 22 millimetres, because this range represents the moment when eggs become fully developed and suitable for extraction.
Your doctor will adjust your medication dosages according to the results of these tests. The system operates in a flexible manner, which adjusts to your requirements while preventing both insufficient stimulation through reduced egg production and excessive stimulation through increased egg production, which may lead to OHSS.
Your doctor will instruct you to perform a trigger injection after your follicles have achieved their target size, which ranges from 17 to 22 millimetres. The shot uses human chorionic gonadotropin (hCG) or a GnRH agonist to start the final stage of egg development, which occurs inside the follicles.
The timing of the trigger shot represents the most important choice during an IVF cycle because it depends entirely on the results from the ultrasound examination. If the trigger occurs too soon, then the eggs will not reach their complete development stage, while waiting too long results in follicles becoming overly developed and breaking before the retrieval process begins.
The timing for egg retrieval in IVF occurs exactly 34 to 36 hours after the trigger injection because scientists have determined this time frame through precise calculations.
The medical staff conducts the IVF egg retrieval process by using ultrasound equipment as part of a continuous fertility ultrasound procedure to monitor their work. Your specialist uses a transvaginal ultrasound probe with a fine needle attached to locate each follicle with accuracy and aspirate the fluid containing the egg.
The real-time ultrasound guidance system enables the retrieval procedure to maintain both its safety and its operational efficiency. The system enables the doctor to track his movements while he collects mature eggs from the body by steering clear of blood vessels and nearby tissues.
The medical process begins to concentrate on the uterus after egg retrieval operations end. The uterine lining must reach optimal conditions because both fresh embryo transfers and frozen embryo transfers (FET) require this condition to enable successful implantation.
You will take your blood pregnancy test (beta-hCG) approximately two weeks after your embryo transfer. The positive result leads to scheduling an IVF pregnancy confirmation scan between 6 and 7 weeks of pregnancy to confirm a clinical pregnancy through the detection of a heartbeat in the uterine cavity.
Most patients experience strong emotional reactions to this scan because it marks an important achievement. The test results confirm successful embryo implantation and show that initial developmental stages are proceeding as expected.
Your individual protocol, together with your ovarian reactions, determines the required number of monitoring appointments. The following schedule shows the required monitoring procedure that needs to be followed during the entire process:
Most patients undergo between 6 and 10 ultrasound scans during a single IVF cycle. Dr. Aravind's IVF centre schedules its appointments in a way which helps patients maintain their daily activities while ensuring complete appointment coverage.
The process of ultrasound monitoring requires technical skills, yet it needs medical experience for proper execution. The doctor who treats two patients with identical follicle measurements needs to use different methods because the patients' medical history, age, hormone levels and previous menstrual cycles need to be evaluated.
The IVF team at Dr. Aravind's clinic has successfully managed more than 70000 cycles during their three decades of experience, which Dr. Aravind Chander leads as a medical professional with an MS in Obstetrics and Gynaecology and a postdoctoral fellowship in reproductive medicine. The extensive experience of our doctors enables them to handle more than just basic numerical data. Their work involves pattern identification and complication prediction, and they use this knowledge to make critical health decisions that result in positive patient outcomes.
The 75% live birth success rate of our IVF program demonstrates both our laboratory excellence and our effective monitoring system, which ensures precise results. We do not believe in a generic approach because we read each scan with its particular context while bringing in your specific medical needs to guide our treatment choices.
The effectiveness of ultrasound monitoring depends on the quality of its supporting infrastructure and equipment and the skills of its operators. The reputation of Dr. Aravind's IVF derives from three main foundation elements, which show our achievements.
Our team provides new treatment methods that combine medical expertise with compassionate care to assist you at any stage of your fertility journey after prior failed attempts at other centres.
The IVF process uses ultrasound monitoring, which remains an essential yet unnoticed component that ensures successful outcomes. The system enables doctors to execute complicated hormonal treatments through its capability to control treatment progress during live sessions, which enhances their chances of successful parenthood.
Every scan at the clinic serves an essential purpose, which starts with the initial baseline scan that establishes your current condition and continues to the endometrial evaluation, which determines your uterine capacity to receive an embryo. The team at Dr. Aravind's IVF Fertility and Pregnancy Centre takes their duty to the public with deep dedication. The team assesses every image through detailed examination. The results from your examination lead to your treatment plan. Each step contributes to improving the IVF success rate in India and achieving positive outcomes.
You can contact us at +91 90 2012 2012 or visit your nearest Dr. Aravind's IVF centre if you want to know more about IVF monitoring or you want to schedule a meeting with our fertility experts.
Most patients undergo 6 to 10 ultrasound scans during a single IVF cycle, including baseline, stimulation monitoring, egg retrieval, and pregnancy confirmation scans.
The trigger shot timing is crucial because it ensures eggs reach full maturity. Triggering too early or too late can reduce egg quality and affect IVF success rates.
An endometrial thickness of 7–10 mm with a trilaminar appearance is considered optimal for successful embryo implantation.
Yes, ultrasound-guided egg retrieval is a safe and precise procedure. It allows doctors to accurately collect eggs while avoiding nearby tissues and blood vessels.
Pregnancy is first confirmed through a beta-hCG blood test about 14 days after embryo transfer, followed by an ultrasound at 6–7 weeks to detect a heartbeat.