He visits the gym four times each week. His blood pressure measurement matches the ideal medical standard. His eating habits, sleeping patterns and his yearly medical examination always produce excellent health results. He displays perfect health through all visible indicators of his well-being. Yet, despite appearing as a healthy man infertility can still be a reality, and he and his partner have spent years trying to conceive, which still remains unfulfilled. This situation exists as a real experience for millions of men who live across the globe.
Society fails to recognize the widespread occurrence of male fertility problems that exist throughout the population. The World Health Organization reports that male factors lead to approximately 50 percent of worldwide infertility cases. The existing stigma about this issue and the common belief that active men with good health always possess fertility, which exists, creates a situation that prevents many men from obtaining medical assistance until their chances for recovery have decreased.
The article investigates, from the start to the end, how men's external health appearance does not determine their capacity for reproduction through an explanation of three factors that create fertility issues and three modern medical treatments, including IVF for male infertility.
Health measurements depend on visible characteristics, which include body weight, physical fitness and presence of chronic conditions and overall energy levels. The indicators show our metabolic and cardiovascular condition, but they provide no information about how sperm manufacturing works, how body hormones function or how male reproductive systems operate at their most fundamental level.
Sperm production occurs in the testes through a biological mechanism known as spermatogenesis, which operates under strict biological controls. The process functions according to its own standards because it responds to various hormonal, temperature, oxidative stress and genetic factors. A man can have strong physical health, yet his sperm count remains low while his sperm appear abnormal and fail to achieve the necessary swimming speed for successful egg fertilization, often without any low sperm count symptoms. The three conditions create internal symptoms that do not produce external signs that can be observed.
The central paradox that most men facing male infertility discover as their most surprising discovery operates without any visible manifestations. The situation includes no pain, no fever and no visible indicators. The only way to know is through a sperm quality test near me, and that is precisely why many cases go undetected until a couple has been trying to conceive for a year or more.
The initial step to solving male infertility problems requires researchers to find its underlying causes. Healthy men who face infertility problems have two primary medical conditions that make them unable to conceive.
A normal sperm count requires a minimum of 15 million sperm to exist in each millilitre of semen. The medical condition known as oligospermia occurs when sperm count drops below this specific threshold. The medical term azoospermia describes cases where no sperm exists in the male reproductive system, requiring advanced azoospermia treatment India options. Many men remain unaware of their existence because both conditions operate without showing any obvious symptoms.
Oligospermia results from three main factors, which include hormonal imbalances, reproductive tract blockages and testicular disorders. Men who experience excessive heat exposure, frequent hot tub use and tight clothing must understand that these activities will lead to temporary decreases in sperm production. The good news is that with the right diagnosis and treatment, sperm counts can often be improved.
Sperm need to maintain an adequate number during the fertilization process because their movement needs to stay functional. Motility refers to the sperm's capacity to swim forward through the female reproductive tract and reach the egg. Sperm with poor motility, a condition called asthenospermia, cannot complete this journey successfully, regardless of how many there are.
Motility problems arise because of oxidative stress, together with nutritional deficiencies, which affect zinc, selenium and antioxidant levels and infections and sperm structural abnormalities. A man with perfect physical health can carry sperm that simply cannot swim well enough to achieve fertilization.
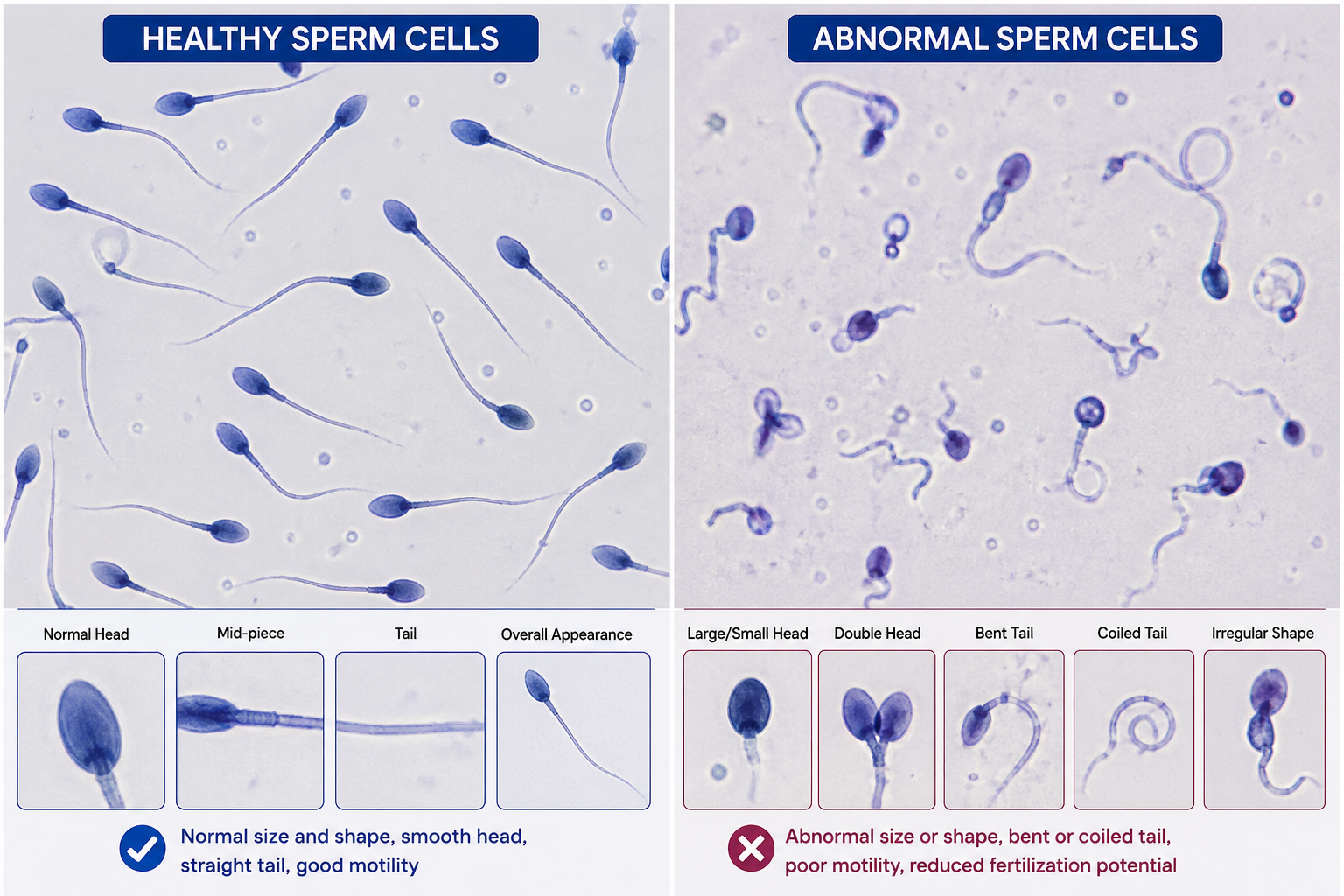
Sperm morphology describes how sperm cells appear in their size and shape characteristics. The typical healthy sperm cell presents an oval head, which maintains a smooth surface together with a tail that exhibits proper construction and length. When more than half of the sperm exhibit abnormal shapes, which include misshapen heads, kinked tails and mid-piece defects, their ability to fertilize decreases by a major percentage. The medical condition called teratospermia represents one of the most common reasons that lead to unknown male infertility.
Abnormal sperm morphology shows no visible symptoms at all. A man needs to undergo sperm testing through a complete semen examination in order to discover whether his sperm contains abnormal shapes. The reason fertility specialists need all-inclusive tests is to establish accurate diagnoses instead of relying on physical exams, which show general health conditions.
A varicocele represents a condition where the scrotal veins experience an expansion that resembles the development of varicose veins that occur in leg veins. The treatment of this condition, strongly linked to varicocele and infertility, represents the most effective solution to male infertility, which scientists have discovered as a primary condition. Approximately 15% of men experience varicoceles, while 35% of men who face primary infertility battle this condition.
The medical condition creates fertility challenges by increasing scrotal temperature, which leads to testicular overheating because sperm development needs temperatures that stay below normal human body heat. Most men with varicoceles experience no pain and have no outward signs of the condition. Medical professionals discover the condition through physical examinations and ultrasound detection, which occurs during fertility assessments.
The brain produces hormones that travel through the body to the testes, which control male fertility. The three hormones follicle-stimulating hormone (FSH), luteinising hormone (LH) and testosterone work together to produce sperm. The hormonal axis maintains sperm production, but any disturbance through pituitary disorders resulting in hormonal imbalance in men fertility, thyroid dysfunction, stress, steroid use or obesity will lead to a significant decrease in sperm production.
Many men who use anabolic steroids for bodybuilding purposes face severe damage to their fertility, even though they maintain a highly developed physical appearance. The body reacts to exogenous testosterone through a complete hormonal signal shutdown, which causes testicular control loss that results in major decreases to sperm production or complete sperm production cessation.
Some genetic conditions directly impact male reproductive ability, whereas they do not produce any visible signs of health issues. Male infertility results from Klinefelter syndrome (XXY chromosomal pattern) and Y-chromosome microdeletions and cystic fibrosis gene mutations. A male who carries this genetic variant will show complete health, but he needs genetic testing to determine his fertility potential.
Leading fertility centres now include genetic evaluation in their standard fertility assessments when normal semen analysis results fail to enable conception.
The reproductive system experiences damage through sexually transmitted infections and various bacterial and viral infections, which result in the formation of scar tissue and blockage of sperm transportation pathways from the testes to the urethra. Mumps orchitis serves as a classic example of a condition that leads to permanent sperm production loss in men who experience its effects without any continuing symptoms.
The immune system creates problems for the body in certain situations. The body develops anti-sperm antibodies, which make it treat its own sperm as if they were outside invaders. The body develops this type of infertility through three medical conditions, which produce no visible symptoms except for the inability to become pregnant.
Certain lifestyle practices decrease fertility in men who otherwise appear healthy. One of the most overlooked factors is stress and male fertility, where chronic stress reduces testosterone, and sperm quality is maintained through healthy lifestyle habits. The following health practices create harmful effects on male fertility:
The gradual and hidden effects of these factors create a situation where men cannot assess their fertility status through daily physical sensations.
The social stigma of male infertility affects South Asian cultures, which spread throughout various regions of the globe. Many men believe that a fertility diagnosis reflects their masculine identity and sexual potency and their value as a romantic partner. The cultural environment creates barriers that make people wait longer before they start medical assessment, and this waiting period decreases the success rate of medical treatments, which could have helped them. Many men hesitate to consult a male fertility specialist Coimbatore or a nearby fertility expert due to embarrassment or misconceptions.
The medical nature of male infertility should be clarified because it exists as a biological condition that does not define a man's masculine identity. The same way people do not judge men who suffer from hypertension or diabetes, society should not make men with low sperm count or impaired sperm motility feel ashamed about their biological medical condition, which is often treatable.
Dr. Aravind's IVF Fertility & Pregnancy Centre specialists have found that couples who work together to solve male infertility problems achieve better results and maintain better emotional strength throughout their journey.
Male fertility assessment starts with a semen analysis, which functions as a simple non-invasive examination that determines sperm count, motility, morphology and volume and additional sperm characteristics. The test delivers extensive medical insights that serve as the primary method for evaluating male reproductive health.
The initial results will determine which additional tests need to be conducted.
The andrologists and reproductive specialists at Dr. Aravind's IVF perform this evaluation process with precise sensitivity because they want to find the exact problem that will lead to developing the most suitable treatment method for each patient.
Modern Treatments That Offer Real Hope
The field of male infertility treatment has made significant progress since the start of the 21st century. Medical treatments now exist for the majority of couples who experience male factor infertility for their condition.
The structured lifestyle intervention program, which includes dietary improvements, weight management and smoking cessation and targeted nutritional supplementation, shows effectiveness to treat mild to moderate cases through three to six months of treatment.
Targeted hormone therapy serves as a solution to restore the body's natural signalling system, which leads to sperm production when hormonal imbalances create the problem. The treatment method shows high effectiveness for men who suffer from hypogonadotropic hypogonadism because their brains fail to produce sufficient hormonal signals, which should reach their testes.
Surgical Intervention for Varicocele and Obstruction
Varicocelectomy serves as an efficient surgical option that doctors use to treat male infertility through varicocele repair. Research demonstrates that the procedure results in enhanced sperm count, mobility and morphological features, which leads to higher pregnancy success rates. The surgical procedure, which corrects obstructive azoospermia, enables men who meet the criteria to achieve their natural fertility potential.
IUI is a procedure that creates a direct path for sperm to reach the uterus through timed sperm delivery at the peak of ovulation. The treatment serves as a solution for men with mild infertility problems who experience difficulty with sperm movement.
ICSI treatment for low sperm count operates as an advanced IVF technique, which uses an embryologist to select one sperm, which they will inject into an egg. The treatment was created to help men who experience severe infertility problems at high levels of sperm production and with weak sperm movement and who suffer from azoospermia without testicular blockage. ICSI has changed the future possibilities for men who used to have no options to become biological fathers.
The Micro-TESE procedure provides men with non-obstructive azoospermia who do not produce sperm in their ejaculate. The surgeon uses a powerful operating microscope to examine testicular tissue while searching for tiny areas that produce sperm that remain hidden from normal sight. Clinicians can use any collected sperm to proceed with an ICSI procedure. The method has restored reproductive chances for men who had been told they would never regain fertility.
Medical guidelines specify that couples should obtain a fertility assessment after 12 months of having unprotected sex without becoming pregnant or after 6 months when the female partner exceeds 35 years of age. The following conditions require assessment before the established time frame:
The act of seeking assistance demonstrates your strength because it helps you build better prospects for your life. The medical field provides more treatment possibilities when doctors confirm a diagnosis at an earlier time.
The main character of male fertility problems exists in absolute silence because this particular silence creates both its most challenging aspect and its most vital component. Most men remain unaware of their treatable condition because the symptoms remain hidden and the illness shows no impact on their daily life, and because society fails to associate male health with sperm production and hormonal levels.
Modern reproductive medicine has developed more diagnostic and treatment options to solve male infertility problems than at any time in its history. The path from diagnosis to parenthood now offers greater accessibility than all previous times because semen analysis provides basic testing while micro-TESE and ICSI deliver advanced diagnostic methods. Consulting a qualified male fertility specialist Coimbatore or visiting the best IVF centre Tamil Nadu can provide clarity, diagnosis, and a clear path toward parenthood.
Men who look and feel healthy but experience difficulty with conception should not let their physical appearance stop them from searching for answers. Specialists require a consultation as their first step in the process. You can begin to gain control over your upcoming path when you acquire knowledge about current circumstances.
Yes. Physical fitness and general health do not reflect sperm quality. A man can look completely healthy but still have issues like low sperm count, poor motility, or abnormal morphology.
Common causes include low sperm count (oligospermia), poor sperm motility (asthenospermia), abnormal sperm shape (teratospermia), varicocele, hormonal imbalances, genetic factors, and infections.
The primary test is a semen analysis, which evaluates sperm count, motility, and morphology. Additional tests may include hormone analysis, ultrasound, genetic testing, and sperm DNA fragmentation tests.
Yes. Stress, smoking, alcohol, poor diet, environmental toxins, and heat exposure can all negatively impact sperm quality without obvious symptoms.
In many cases, yes. Treatments range from lifestyle changes and medications to advanced options like IUI, IVF, ICSI, and Micro-TESE.