The decision to start something better through IVF marks the beginning of parenthood, which requires extreme bravery because it creates deep emotional turmoil for couples. Our team at Dr. Aravind's IVF Fertility & Pregnancy Centre provides support to numerous couples who need assistance throughout their complete path, which they will follow to achieve their various goals. Body Mass Index, commonly known as BMI, stands as one of the most important yet neglected elements that determine BMI and IVF success rates in fertility procedures.
Your weight has a crucial impact on your ability to reproduce, which can either help you succeed or make everything harder for you, whether you are starting to learn about fertility treatments or already progressing through your IVF process. This article provides an analysis of how BMI affects IVF success rates in women and explains its impact on each treatment stage while presenting effective methods that improve your chances of becoming pregnant successfully.
Body Mass Index represents a basic mathematical calculation that connects your body weight to your body height. Your weight in kilograms gets divided by the square of your height in meters to compute this measurement. A woman who weighs 65 kilograms and stands 1.65 meters tall would have a BMI of approximately 23.9, which falls within the normal range and supports better body weight and fertility outcomes.
Healthcare providers around the world use BMI as a quick, accessible screening tool to categorise weight status. The test does not provide direct body fat percentage measurements, but it accurately shows whether someone belongs to the underweight, healthy weight, overweight, or obese categories.
The standard classifications used in clinical practice are as follows:
Research shows that South Asian populations, which include patients from Tamil Nadu, Kerala, Karnataka and other states where Dr. Aravind's IVF operates, start experiencing health problems because of excess weight at lower BMI levels than other populations. Many specialists, therefore, apply a more conservative ideal BMI for IVF success in India, ranging from 18.5 to 22.9 when evaluating fertility outcomes for Indian patients.
The connection between body weight and reproductive health exists because of biological factors. Adipose tissue functions as an active metabolic organ that generates and controls hormonal activities, including oestrogen production. The body experiences major disruptions to its hormonal balance when body fat percentage exceeds or falls below optimal levels, which leads to severe effects on fertility.
In women who are overweight or obese, their body produces excess oestrogen because their excess fat tissue creates more oestrogen than normal. The hormonal excess creates an imbalance that prevents natural brain-ovary communication from occurring. The pituitary gland will not produce enough follicle-stimulating hormone (FSH) and luteinising hormone (LH) to induce ovulation.
The main reason women with high BMI experience irregular or absent periods because their hormonal cascade pathways have been disrupted. Natural conception becomes much harder when women do not ovulate because their fertility treatments become less effective.
PCOS represents one of the main causes of infertility that affects women during their reproductive years, while also establishing a proven connection to body weight. Women with PCOS show insulin resistance because their body cells fail to respond properly to insulin. The body reacts by increasing insulin production, which leads to excessive insulin levels that cause the ovaries to generate additional male hormones. These androgens stop normal follicle maturation as well as ovulation from occurring.
Ineffective insulin management results from PCOS, which develops based on a person's body mass index. Weight gain becomes problematic because it worsens insulin resistance while also disrupting hormonal balance. Multiple clinical studies demonstrate that women with PCOS experience better ovulation patterns when they achieve weight loss between five and ten percent because this improvement increases their chances of natural conception and assisted reproductive success.
Underweight individuals face their own serious challenges, which impede their ability to conceive a child. When body fat levels drop below a certain threshold, the body interprets this condition as either nutritional deprivation or stress. The brain's hypothalamus centers which manage hormonal signal distribution, will stop or decrease their GnRH hormone production. The pituitary gland needs GnRH to produce FSH and LH, which prevents ovulation from occurring.
The medical condition known as hypothalamic amenorrhea occurs most frequently in women who maintain extremely low body weight, engage in excessive physical activity, and are in recovery from eating disorders. The body of underweight women uses menstruation cessation as a method to save energy while it protects itself from pregnancy requirements during times of food scarcity.
The IVF treatment process for women consists of multiple steps, which require proper hormonal levels to maintain their operational effectiveness. An abnormal BMI can create difficulties that emerge at various stages throughout this process.
The first major phase of an IVF cycle begins when doctors use injectable gonadotropin hormones to stimulate the ovaries for multiple follicle development. Women with a higher BMI require their medications in much larger quantities to achieve the same level of ovarian response that normal BMI women reach with standard treatment. The body metabolises and distributes fertility drugs differently because excess body fat exists, which leads to reduced drug effectiveness through lower bloodstream concentrations.
Longer stimulation times result from higher medication needs, which also drive up costs and create extra risks for side effects. The ovaries of underweight women produce follicles, but these follicles display suboptimal quality because of their hormonal deficiency, which causes their stimulation response to show unpredictability.
The success of an IVF cycle depends on multiple critical factors, but the quality of retrieved eggs stands as a major deciding factor. Eggs which develop within a hormonally deficient environment show increased chances of chromosomal defects, diminished fertilization ability and decreased development potential after fertilization. Researchers have discovered through various studies that women with a BMI above 30 produce fewer mature eggs per IVF cycle and that those eggs are more likely to be of lower quality compared to eggs retrieved from women with a normal BMI.
Obese and overweight individuals show higher levels of inflammatory markers, which can create a direct impact on the follicular fluid environment that supports egg maturation. High-quality eggs, which provide embryos with their best chance to develop and implant, face additional obstacles because of this situation.
The success of fertilization does not prevent BMI from affecting the results of embryo development. Research has shown that embryos that originate from high BMI women show decreased overall blastocyst development. The implantation process begins when a viable embryo attaches itself to the uterine lining.
Successful implantation of the embryo requires the uterine endometrium to achieve three conditions, which include appropriate receptiveness, high vascularization and complete hormonal readiness. The combination of excess oestrogen from adipose tissue and increased inflammatory cytokines leads to changes in uterine lining receptivity, which decreases the chances of successful embryo implantation.
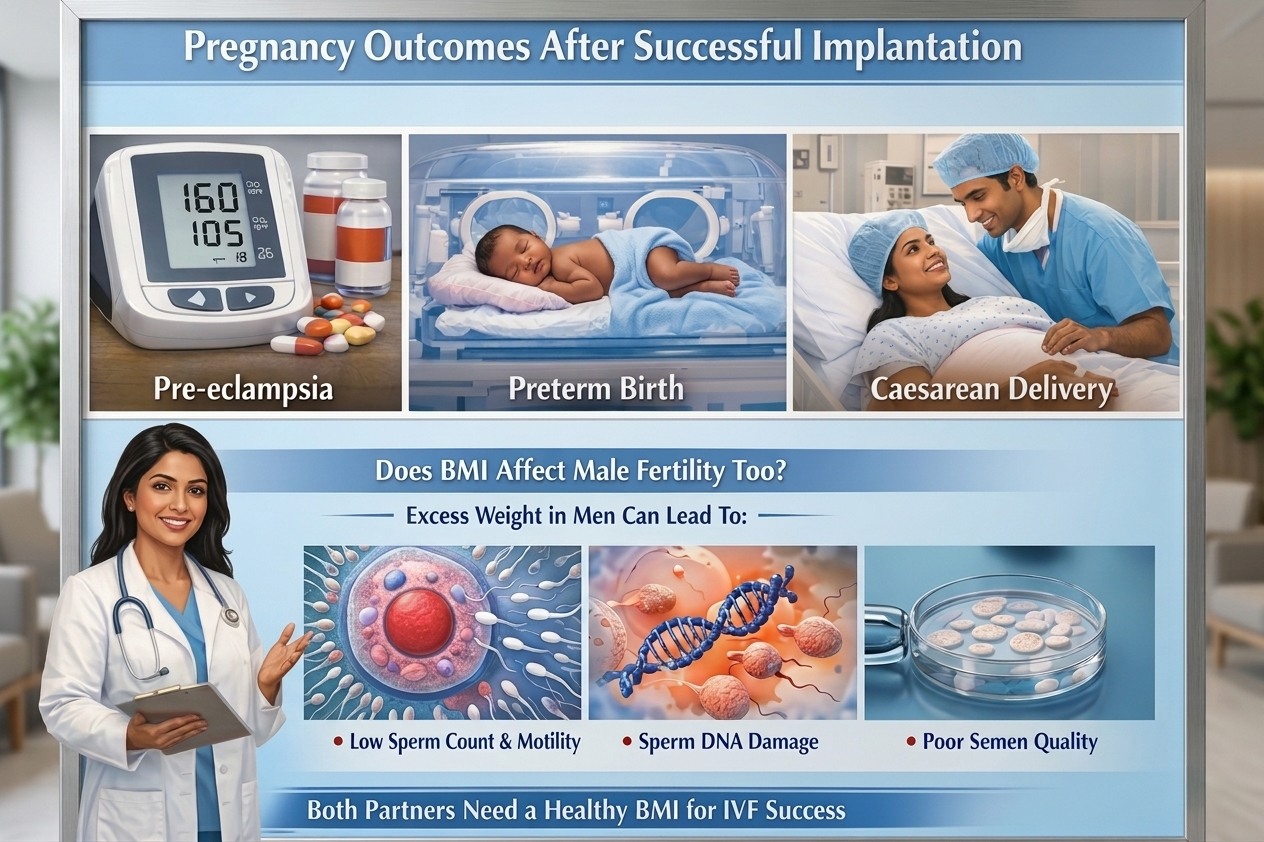
The effects of BMI continue to affect women until they achieve a positive result from their pregnancy test. Women who conceive through IVF with a BMI outside the healthy range face a higher risk of pregnancy complications, which include gestational diabetes, pre-eclampsia, preterm birth and the need for caesarean delivery. The patient population in South India faces a higher gestational diabetes risk because the condition occurs more frequently than in Western populations, even among individuals with lower BMI measurements.
Underweight women who become pregnant face higher risks of delivering low-birthweight infants and experiencing preterm labour. Women who achieve optimal BMI levels before and during their pregnancy period help improve maternal and infant health outcomes.
Research and clinical discussions about IVF and BMI mainly study women, but researchers need to acknowledge that male BMI affects both their fertility and IVF outcomes. Men who carry excessive body weight experience hormonal changes that stop them from producing healthy sperm. Men store body fat in their abdominal area, which converts their testosterone levels into oestrogen through the process of aromatisation. Increased oestrogen levels in males result in suppressed FSH and LH production, which causes decreased testosterone levels and leads to diminished sperm production capacity. Research has established that men with high BMI levels experience decreased sperm counts and lower sperm motility while showing increased DNA fragmentation in sperm and resulting in worse semen quality.
The direct sperm injection process used during IVF with ICSI at all Dr. Aravind's IVF centres requires optimal sperm quality for successful fertilization. Sperm with elevated DNA fragmentation rates result in lower chances of creating viable embryos, therefore both partners should maintain healthy BMI levels for maximum fertility potential.
The positive fact shows that even slight BMI changes can lead to significantly better results from IVF treatments. At Dr. Aravind's IVF, our team of fertility specialists, gynaecologists and nutritional counsellors work together to assist patients in achieving their ideal weight before they start or continue their IVF process. Here is a structured approach to getting there.
Your health needs to be assessed completely before you start any fertility treatments. The evaluation process at our centres requires you to undergo a BMI assessment and complete hormonal blood testing, thyroid function tests and insulin resistance testing and provide your menstrual cycle history. Your doctor needs your current BMI status information because it shows how your body functions to create a customized treatment strategy and set precise treatment objectives.
The human body requires food, which consists of essential nutrients for its proper functioning, but crash diets and extreme calorie restrictions do not benefit people who need to prepare their bodies for in vitro fertilization procedures. The practice of extreme calorie restriction results in both a decrease in AMH hormone levels and a complete depletion of essential micronutrients, while the body enters a condition of stress, which damages its ability to reproduce.
The most efficient method requires a balanced eating plan which provides nutrient-dense foods that create a small caloric deficit while the body receives sufficient folate, iron, omega-3 fatty acids, vitamin D and antioxidants. Research shows that the Mediterranean-style diet, which emphasizes whole grains, legumes, vegetables, lean proteins, healthy fats from olive oil and nuts, while minimizing processed foods, leads to better IVF results and higher egg quality. Our nutritional counsellors can assist you in creating this dietary approach, which will respect your cultural food traditions and your personal dietary habits.
Insulin sensitivity improvement occurs through physical activity, which helps people achieve their ideal body weight while reducing their body fat. The specific exercise type, together with its intensity level, affects your IVF preparation and treatment process. People generally find moderate exercises, which include brisk walking, swimming, cycling and yoga, to be beneficial. Women who have enlarged ovaries should avoid intense high-impact training during their stimulation cycle because it raises their risk of experiencing ovarian torsion.
You should complete 150 minutes of moderate physical activity each week during the three months before your IVF cycle. Women who currently weigh too little and work out too much need to decrease their workout effort, while they should increase their food consumption according to medical advice.
The treatment plan for women with PCOS and insulin resistance requires both medical approaches and lifestyle modification. The medication metformin, which enhances insulin sensitivity, is a standard treatment in fertility management that has demonstrated improvements in both ovulation rates and IVF success for women with PCOS. The combination of myo-inositol and D-chiro-inositol for inositol supplementation has demonstrated effective results in enhancing insulin sensitivity and improving egg quality.
The specialist at Dr. Aravind's IVF will assess your medical situation through test results and medical history to determine which treatments are suitable for you.
The process of achieving sustainable weight changes needs an extended duration to produce results because quick weight loss should be avoided. The majority of fertility experts advise patients to achieve their optimal body mass index and maintain that weight for a minimum period of two to three months before starting ovarian stimulation because the body requires this time to improve its metabolic and hormonal functions, which will lead to better reproductive health results after three months.
The clinical team at Dr. Aravind's IVF Fertility and Pregnancy Centre uses BMI measurements to assess patients before they start their medical treatments. The clinic evaluates patients with body mass index (BMI) measurements because they provide important information about their treatment needs that exist beyond standardized BMI treatment thresholds. The specialists at our organization create personalized treatment plans that use BMI measurement together with age, ovarian reserve, hormone levels, partner fertility information and patient history of medical procedures.
Our organization exists to assist couples in finding the safest method that leads to successful parenthood. We establish a pre-treatment optimization program for patients who present with major BMI issues, which must be completed before we start their ovarian stimulation. Healthier outcomes occur when we invest time into preparing our work because it decreases the chances of complications that might affect both mothers and their newborns.
Dr Aravind's IVF clinic offers 30 years of experience and 70000 completed IVF treatments, which lead to 75 percent live birth success rates. Our Coimbatore, Chennai, Bangalore, Salem, Erode, Tiruppur, Hosur, Palakkad and Kozhikode centres maintain a staff of dedicated fertility specialists and embryologists who provide complete support to clients throughout their treatment.
The relationship between BMI and IVF success is clear, compelling, and clinically significant. The most effective investment for your fertility journey exists in the steps that you should take to achieve a healthy BMI range before your IVF cycle begins.
Dr. Aravind's IVF Fertility and Pregnancy Centre provides you with complete assistance to prepare for your parenthood journey through their advanced medical services and dedicated staff who support your dreams of becoming a parent. Understanding how BMI affects IVF success rates in women helps you take proactive steps toward improving outcomes.
You can schedule a consultation at our South India and Sri Lanka centres to discuss your BMI with our fertility specialists and learn how it impacts your IVF success chances. Your journey deserves the best possible beginning because every journey is different from others.
The ideal BMI for IVF success in India is typically between 18.5 and 22.9 for optimal fertility outcomes.
Yes, losing even 5–10% of body weight can significantly improve ovulation and IVF outcomes.
Yes, low BMI can disrupt hormones and reduce ovulation, affecting fertility treatment success.
High BMI is linked to poor egg quality and lower fertilization rates in IVF.
Yes, high BMI in men can reduce sperm quality and affect fertilization outcomes.